Familial hemophagocytic lymphohistiocytosis in a newborn presenting with recurrent fever and thrombocytopenia: a case report
Introduction
Familial hemophagocytic lymphohistiocytosis (HLH) is a rare and potentially fatal disease with major difficulties of diagnosis and treatment, especially in the neonatal period (1-3). Early diagnosis and early treatment of HLH improves patients’ outcomes. Herein, we present a Familial HLH case and discuss the differential diagnosis and the cutting edge opinions of treatment by the experts in this area.
Case presentation
A 20-day-old male patient was admitted due to “fever for 1 day accompanied by thrombocytopenia”. The infant was born at 37+4/7 weeks gestational age to a G2P2 mother via cesarean section due to a scarred uterus. The pregnancy was uncomplicated except for maternal hypothyroidism in the third trimester. There was no parental consanguinity. His birth weight was 2,700 g and Apgar scores were 9 and 9 at 1 and 5 minutes respectively. He had no history of respiratory distress, and amniotic fluid, umbilical cord, and placenta showed no obvious abnormality. He was fed both breast milk and formula since birth. One day before admission (19 days after birth), he had a fever (38 °C) which normalized after physical cooling. He had no shortness of breath, convulsions, irritability, staring episodes, appetite change, or decreased movement. He passed 8–10 yellow greasy stools per day, and his urine volume was normal. He passed the newborn screening and hearing screening. He received hepatitis B and BCG vaccination, and there was no notable abnormality at the BCG vaccination site.
At presentation, his routine blood test showed: WBC 14.8×109/L, abnormal lymphocyte cells 30%, hemoglobin 113 g/L, and platelets 63×109/L. He was admitted to our unit for “fever and thrombocytopenia”.
The child’s elder brother died 1 month after birth. The disease history of his brother was as follows: the child was born in 2012; 8 days after his birth, he was admitted in a local hospital due to “diarrhea for 5 days, with fever for 4 days”. Diarrhea occurred 4 days after birth, accompanied by fever. Three routine blood tests revealed thrombocytopenia (the lowest amount: 8×109/L), along with repeated fever. Eight days after birth he was admitted to a hospital. Upon admission he was treated with cefodizine, cefoperazone, and meropenem to fight against infection; also, symptomatic treatment was applied for thrombocytopenia and coagulation disorders. After admission, the child had recurrent high fever and abdominal distention. Twelve days after admission, he suffered from bloody stool; abdominal X-ray revealed intestinal perforation, which was treated by double-lumen enterostomy. After the surgery, the child still had abdominal distention and severe infection-related symptoms, along with persistent fever, low platelet count, enlarged liver and spleen, and abnormal coagulation function. These conditions did not respond to symptomatic treatments with various antibiotics and blood products. He died 34 days after admission when his heart rate could not be maintained.
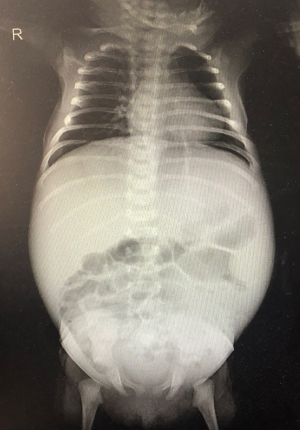
The present patient was active and alert at admission, with general reactions. He had a slightly pale complexion, his skin was not obviously jaundiced, and he had no rashes, bruising, or petechiae. His anterior fontanelle was flat and soft, the sclera was not jaundiced, and his neck was soft. Respiratory sounds were rough in both lungs, and no obvious dry or wet rales were heard. The heart sounds were strong, and there were no obvious murmurs in the precordial area. The abdominal area was soft, the liver and spleen were not large initially, but gradually enlarged during his hospital stay. The lab results and X-ray as follows: Table 1 and Figure 1.
Table 1
| Items | Reference value | At admission | Three days after admission | One week after admission | Ten days after admission |
|---|---|---|---|---|---|
| Hemoglobin (g/L) | 150–230 | 94 | 81 | 87 | 86 |
| Hematocrit (%) | 55.4–60.2 | 28 | 23.2 | 25.0 | 26.10 |
| White blood cells (WBC) (×109/L) | 10–24 | 16.1 | 14.7 | 5.5 | 6.1 |
| Neutrophils (%) | 50–70 | 20.0 | 15.0 | 6.8 | 8.5 |
| Lymphocytes (%) | 30–40 | 50.0 | 60.0 | 74.2 | 4.7 |
| Monocytes (%) | 3–8 | 10.0 | 10.0 | 17.8 | 12.5 |
| Eosinophils (%) | 0.5–5 | 0.0 | 0.0 | 0.5 | 0.2 |
| Basophils (%) | 0–1 | 0.0 | 0.0 | 0.7 | 1.5 |
| Abnormal lymphocytes cells (%) | 0–5 | 20 | 15 | Occasional seen | |
| Platelets (×109/L) | 100–400 | 50 | 23 | 19 | 32 |
| C-reactive protein (mg/L) | <8 | 8 | 29 | <8 | 8 |
| Alanine aminotransferase (IU/L) | 0–40 | 77 | 51 | ||
| Aspartate aminotransferase (IU/L) | 25–75 | 132 | 62 | ||
| Total protein (g/L) | 60–83 | 44.5 | 59 | ||
| Albumin (g/L) | 35–55 | 31.4 | 34 | ||
| Globulin (g/L) | 20–30 | 13.1 | 25 | ||
| Creatinine (μmol/L) | 27–66 | 16.0 | 15 | ||
| Urea (mmol/L) | 2.5–6.5 | 1.90 | 3.5 | ||
| Uric acid (μmol/L) | 90–420 | 186 | 154 | ||
| Creatine kinase (IU/L) | 42–383 | 38 | 34 | ||
| Creatine kinase isoenzyme (IU/L) | 25–200 | 42 | 39 | ||
| Triglycerides (mmol/L) | 0.56–1.7 | 2.35 | |||
| Potassium | 3.5–5.5 | 4.10 | 4.7 | ||
| Sodium | 135–150 | 132 | 129 | ||
| Calcium | 2.25–2.75 | 2.3 | 2.11 | ||
| Chlorine | 96–108 | 99 | 96 | ||
| Blood ammonia (μmol/L) | 72 | ||||
| Activated partial thromboplastin time (APTT) (s) | 26–40 | 46.6 | 81.2 | ||
| D-dimer (mg/L) | 0–0.5 | 2.04 | 0.89 | ||
| Fibrinogen (g/L) | 2–4 | 1.30 | <0.6 | ||
| International normalized ratio (INR) | 0.8–1.2 | 1.33 | 6.00 | ||
| Fibrin degradation products (FDP) (μg/mL) | 0–5 | 6.97 | 2.83 | ||
| Prothrombin time (s) | 11–14.5 | 16.7 | 54.5 | ||
| Prothrombin time activity (%) | 80–120 | 64 | 13 | ||
| Thrombin time (s) | 11–14.5 | 20.6 | 86.5 | ||
| IgA (g/L) | 0.004–0.017 | 0.03 | |||
| IgG (g/L) | 6.46–17.74 | 4.20 | |||
| IgM (g/L) | 0.05–0.27 | 0.17 | |||
| IgE (g/L) | <100 | <2.0 | |||
| C3 (g/L) | 0.67–1.76 | 1.07 | |||
| C4 (g/L) | 0.1–0.4 | 0.28 | |||
| CH50 | 23–46 | 34 | |||
| PCT (ng/dL) | <0.05 | 0.43 | |||
| CD16+CD56+ (%) | 11–23 | 8.51 | |||
| CD19+ (%) | 14–21 | 5.18 | |||
| CD3+ (%) | 64–73 | 85.69 | |||
| CD4+ (%) | 29–36 | 24.76 | |||
| CD8+ (%) | 24–34 | 61.44 | |||
| Erythrocyte sedimentation rate (ESR) | 0–21 | 2 | |||
| Ferritin (ng/mL) | 26.08–287.5 | >2,000 | |||
| Carcinoembryonic antigen (ng/mL) | <5.0 | 3.94 | |||
| α-fetoprotein (AFP) (ng/mL) | <164,000 | 757.70 | |||
| Herpes simplex virus I/II IgM | Negative | Negative | |||
| CMV IgM | Negative | Negative | |||
| Rubella virus IgM | Negative | Negative | |||
| Toxoplasma gondii IgM | Negative | Negative | |||
| Parvovirus IgM | Negative | Negative | |||
| Epstein-Barr virus (EBV) DNA | Negative | Negative | |||
| EBV inside WBC | Negative | Negative | |||
| Herpes simplex virus DNA | Negative | Negative | |||
| Enterovirus DNA | Negative | Negative |
iMDT discussion
Discussion among pediatricians of Children’s Hospital of Fudan University
The 20-day-old male was presented with recurrent fever accompanied by reductions in platelets, hemoglobin, and neutrophils and abnormal lymphocyte proliferation. The conditions responded poorly to symptomatic infusion of blood products, and progressive enlargements of liver and spleen were observed. The differential diagnoses were as follows.
(I) HLH
HLH was considered since the child had fever, reductions in platelets, hemoglobin, and neutrophils, low fibrinogen, hepatosplenomegaly, increased ferritin level, slightly decreased NK cell viability, and increased triglyceride level. HLH can be either primary or secondary. The primary HLH is mainly familial, caused often by autosomal recessive or compound heterozygous mutations, whereas secondary lesions are often caused by factors such as infection, tumor, and medication. In our current case, test for EB virus showed negative result, and bone biopsy excluded the possibility of hematological malignancy. Similar disease history was found in the child’s elder brother, suggesting the possibility of familial HLH.
(II) Primary immunodeficiency
Immune deficiencies in the child included decreased NK cell and B cell functions and T cell dysfunction, and the possibility of primary immunodeficiency could not be ruled out. However, further typing and detection of immune functions showed no notable abnormality, and chimerism detection also revealed no obvious chimerism, which means no special maternal cells found in the patient. Therefore, a clinical diagnosis of primary immunodeficiency could not be made.
(III) Eczema-thrombocytopenia-immunodeficiency syndrome
This disease is clinically characterized by eczema, immune deficiency, and thrombocytopenia, with WAS protein gene mutation as the etiology of the disease. Male children are more susceptible to this disease, showing recurrent infections and thrombocytopenia. In our current case, however, the child did not have eczema, platelet count did not remarkably decrease, and WAS protein was within the normal range. Therefore, a diagnosis of eczema-thrombocytopenia-immunodeficiency syndrome could be ruled out.
Final diagnosis of this patient was HLH. After admission, ampicillin combined with ceftazidime was used to fight against infections. The child suffered from recurrent fever after admission, with the peak temperature ranging 37.5–38 °C, and the liver and spleen progressively enlarged. The patient had reduction in platelets, hemoglobin, and neutrophils, increased ferritin, low fibrinogen, and increased triglyceride level. Bone marrow biopsy revealed hemophagocytic cells. Clinical exome sequencing showed complex heterozygous/suspicious variants of STXBP2 gene. Also based on the child’s family history, there was a high possibility of familial HLH. The child was treated with methylprednisolone, dexamethasone, and etoposide. After repeated infusion with red blood cells, platelets, plasma, cryoprecipitate, and gamma globulin, cefepime, imipenem, and vancomycin were applied as anti-infective agents, along with fluconazole for preventing fungal infection. The child suffered from repeated acidosis and fluctuation of blood oxygen during the treatment course. Two months after admission, tracheal intubation could not be maintained due to his poor blood oxygen. Testing showed metabolic acidosis and hyperlactatemia. The parents abandoned treatment considering the poor prognosis.
Validation tests in his parents confirmed the diagnosis of familial HLH type 5 (caused by STXBP2 mutation), with one heterozygous variant carried by each parent (mother: NM-006949:exon 14: c.1246+5G>A; father: NM-006949:exon 15: c.1254_1257delTAAG). Parents were advised to seek genetic counseling.
Several issues regarding the management of this patient were further discussed as follows
Question 1: this HLH patient was deteriorating rapidly after admission to our hospital, and we treated this baby with HLH-specific medicines, dexamethasone and etoposide. But this baby was still unstable and acutely ill. So the question is what other treatment we could try when patients do not show a response to the initial HLH specific treatment (dexamethasone and etoposide)?
Expert opinion 1: Dr. Christopher Dandoy & Dr. Erika L. Stalets
There is no standard definition of refractory HLH. However, Marsh et al. (4) defined refractory HLH as failing to obtain an adequate response to conventional therapy, and Wang et al. (5) described it as the failure to achieve at least a partial response two weeks following standard HLH therapy.
Recently, the Histiocyte Society Salvage Therapy Working Group (4) completed a comprehensive review of the literature to summarize the published experience of reported treatments for patients with refractory HLH. These treatments include Anakinra, an IL-1 receptor antagonist; anti-thymocyte globulin (ATG); alemtuzumab (Campath), an anti-CD52 antibody; and liposomal doxorubicin treatment combined with etoposide and methylprednisolone (DEP). Unfortunately, the data supporting each of these interventions is limited, and it is difficult to conclusively decide which, if any of the available salvage therapies should be employed.
Expert opinion 2: Dr. Blachy Davila Saldana
Unfortunately, this is a very common scenario in the setting of HLH. Results from the HLH 2004 trial (6) show that almost half of all children will not achieve or maintain full resolution of disease with these medications alone. This has led to many attempts at “salvage” therapy. As the disease is so rare, there is scant data to demonstrate what is the best second tier line treatment for the condition. Alemtuzumab has been tried often, as well as anakinra. European groups have attempted ATG as well. JAK inhibitors (ruxolitinib) have also been used to success, mostly in adults. Marsh et al. published a comprehensive summary of this experience (4). Recently, a novel anti-interferon treatment called emapalumab has been approved for primary HLH in Europe and the US, though this is extremely recent so there is little data outside of the original clinical trial.
Question 2: the evidence showed familial HLH patients all require allogeneic hematopoietic cell transplant to attain long-term cure of disease. The question is how early could we start hematopoietic cell transplant in congenital patients?
Expert opinion 1: Dr. Christopher Dandoy & Dr. Erika L. Stalets
Patients with homozygous or compound heterozygous HLH gene mutations should undergo hematopoietic stem cell transplant (HSCT) (1). In patients who require HSCT, such as the one described, transplant should occur shortly after the initial eight weeks of etoposide and dexamethasone treatment. It is important to note, however, that remission of HLH prior to the start of the preparative regimen is associated with less transplant-related mortality (7). Thus, initiation of the preparative regimen should start soon after remission is obtained.
Expert opinion 2: Dr. Blachy Davila Saldana
From what we know of this disease, having an episode of HLH in the setting of known mutations associated with familial disease is associated with an almost 100% chance of recurrence unless definitive therapy is given. Allogeneic transplant remains the only definitive treatment for now. Given the high morbidity and mortality associated with relapsed or refractory disease, we advocate that children with familial HLH should proceed to allogeneic HSCT as soon as clinically possible. However, what data we have does show it is very important to achieve disease control in order to proceed to transplant (akin to obtaining a low MRD before HSCT for leukemias). If this is achieved, age is not a factor; we have transplanted infants down to 4 months of age with success.
Question 3: after HCT, will patients need to be monitored for disease recurrence? If yes, what kind of exams or how often we should use to monitor the patients’ situation? In some extreme cases, is it possible to perform second transplant?
Expert opinion 1: Dr. Christopher Dandoy & Dr. Erika L. Stalets
As stated above, patient who are homozygous or compound heterozygous for HLH gene mutations should undergo HSCT. Further, patients who have a lack of response to initial HLH therapy or have central nervous system involvement should also undergo HSCT in a timely manner (7). Reduced-intensity conditioning regimens for hematopoietic stem cell transplantation has improved survival in hereditary HLH, however, this is at a cost of frequent mixed chimerism (8,9). However, low chimerism is a significant cause for HLH disease recurrence, oftentimes resulting a need for donor lymphocyte infusions (DLI) and/or second allogeneic transplants (8). Providers should follow donor chimerism closely after allogeneic stem cell transplant for HLH, and increases in inflammatory markers, such as ferritin and sIL2r after transplant merits further investigation.
Expert opinion 2: Dr. Blachy Davila Saldana
Yes, disease monitoring is important, and is somewhat dependent on the way transplant is done. Historically, myeloablative transplant in HLH has been associated with a higher risk of mortality. This has led to the use of reduced intensity regimens for this disorder. In the biggest study to date (10), reduced intensity conditioning was associated with much lower transplant- related mortality, but a much higher incidence of graft failure requiring DLI or second HSCT. Given the high mortality with myeloablation, reduced intensity regimens are still more often used for this disease. However, this means that disease monitoring is of paramount importance, as there is a higher need for interventions post HSCT. We do lineage specific chimerism to look at donor percentage in the T cells; data shows that 20–30% donor T cell chimerism is enough to achieve long term cure (8). We will monitor monthly for the first three months’ post HSCT, then proceed to decrease frequency as chimerism stabilizes. If it does drop below 20%, we will consider a second transplant; this is only done with parental request if the child is asymptomatic, but if there is redevelopment of HLH we will proceed to remission and second allogeneic HSCT.
Conclusions
Familial HLH is characterized by recurrent fever, and reductions in platelets, hemoglobin, and neutrophils, and is treated differently from sepsis, or other hematological diseases. Patients with homozygous or compound heterozygous HLH gene mutations should undergo HSCT. And it is very important to achieve disease control in order to proceed to transplant by conventional therapies or trying other salvage medicines.
Acknowledgments
Funding: None.
Footnote
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/pm.2019.09.02). WHZ serves as an unpaid executive editor-in-chief of Pediatric Medicine. The authors have no other conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. All procedures performed in studies involving human participants were in accordance with the Declaration of Helsinki (as revised in 2013). Written informed consent was obtained from the patient for publication of this manuscript and any accompanying images.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Jordan MB, Allen CE, Weitzman S, et al. How I treat hemophagocytic lymphohistiocytosis. Blood 2011;118:4041-52. [Crossref] [PubMed]
- Kostova EB, Beuger BM, Veldthuis M, et al. Intrinsic defects in erythroid cells from familial hemophagocytic lymphohistiocytosis type 5 patients identify a role for STXBP2/Munc18-2 in erythropoiesis and phospholipid scrambling. Exp Hematol 2015;43:1072-6.e2. [Crossref] [PubMed]
- Xu XJ, Wang HS, Ju XL, et al. Clinical presentation and outcome of pediatric patients with hemophagocytic lymphohistiocytosis in China: A retrospective multicenter study. Pediatr Blood Cancer 2017; [Crossref] [PubMed]
- Marsh RA, Jordan MB, Talano JA, et al. Salvage therapy for refractory hemophagocytic lymphohistiocytosis: A review of the published experience. Pediatr Blood Cancer 2017; [Crossref] [PubMed]
- Wang Y, Huang W, Hu L, et al. Multicenter study of combination DEP regimen as a salvage therapy for adult refractory hemophagocytic lymphohistiocytosis. Blood 2015;126:2186-92. [Crossref] [PubMed]
- Bergsten E, Horne A, Arico M, et al. Confirmed efficacy of etoposide and dexamethasone in HLH treatment: long-term results of the cooperative HLH-2004 study. Blood 2017;130:2728-38. [Crossref] [PubMed]
- Wang Y, Wang Z. Treatment of hemophagocytic lymphohistiocytosis. Curr Opin Hematol 2017;24:54-8. [Crossref] [PubMed]
- Hartz B, Marsh R, Rao K, et al. The minimum required level of donor chimerism in hereditary hemophagocytic lymphohistiocytosis. Blood 2016;127:3281-90. [Crossref] [PubMed]
- Marsh RA, Jordan MB, Filipovich AH. Reduced-intensity conditioning haematopoietic cell transplantation for haemophagocytic lymphohistiocytosis: an important step forward. Br J Haematol 2011;154:556-63. [Crossref] [PubMed]
- Allen CE, Marsh R, Dawson P, et al. Reduced-intensity conditioning for hematopoietic cell transplant for HLH and primary immune deficiencies. Blood 2018;132:1438-51. [Crossref] [PubMed]
Cite this article as: Yin R, Wang H, Li Z, Cao Y, Yang L, Wang H, Wu B, Dandoy C, Stalets EL, Saldaña BJD, Wang L, Zhou W. Familial hemophagocytic lymphohistiocytosis in a newborn presenting with recurrent fever and thrombocytopenia: a case report. Pediatr Med 2019;2:49.